A Comprehensive Patient Guide
Obstructive Sleep Apnea (OSA) is far more than snoring—it is a chronic, progressive condition that affects breathing, sleep architecture, cardiovascular health, brain function, and long-term survival.
Today, the management of OSA has entered a new era.
As surgeons and innovators working at the intersection of advanced airway surgery and artificial intelligence, our approach is grounded in precision medicine—leveraging high-resolution imaging, dynamic airway evaluation, and data-driven modeling to design individualized treatment strategies.
We are no longer limited to generalized therapies or "trial-and-error" care. We can now:
- Identify the exact anatomical cause of airway collapse
- Predict which treatments will work before they are performed
- Deliver targeted, multi-level surgical solutions with greater success and durability
This guide will help you understand:
- What OSA is and why it matters
- How it is diagnosed using modern tools and AI
- When surgery becomes the optimal solution
- The full spectrum of advanced surgical options
- What outcomes and recovery you can expect
What Is Obstructive Sleep Apnea?
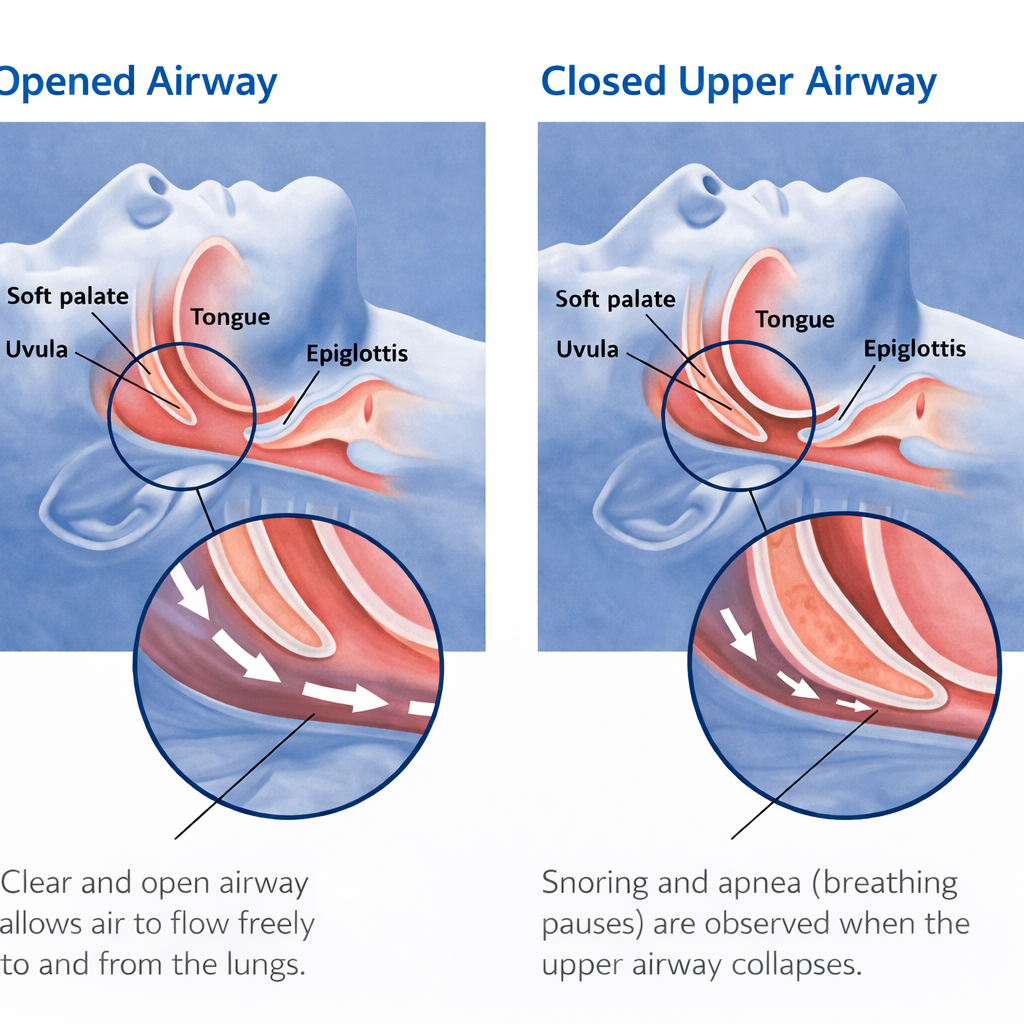
OSA occurs when the airway repeatedly narrows or collapses during sleep, leading to:
- Reduced airflow (hypopnea)
- Complete pauses in breathing (apnea)
These events can occur dozens to hundreds of times per night, fragmenting sleep and placing stress on nearly every organ system.
Common Symptoms
- Loud, habitual snoring
- Witnessed pauses in breathing
- Gasping or choking during sleep
- Excessive daytime fatigue
- Brain fog or impaired concentration
- Morning headaches
- Poor memory and reduced performance
- Mood disturbances (irritability, anxiety, depression)
Why It Matters: Systemic Health Impact
Untreated OSA is strongly associated with:
- Hypertension (often resistant to medication)
- Coronary artery disease and heart attack
- Stroke
- Atrial fibrillation and arrhythmias
- Type 2 diabetes and metabolic dysfunction
- Cognitive decline and increased dementia risk
- Increased perioperative and anesthesia risk
- Reduced lifespan
OSA is not simply a sleep disorder, it is a whole-body disease.
The Modern Diagnostic Approach
Effective treatment begins with accurate, multi-dimensional diagnosis.
1
Sleep TestingDiagnosis is confirmed through objective sleep measurement:
Home Sleep Apnea Testing (HSAT)
- Convenient and increasingly accurate
- Ideal for many patients
- Measures breathing patterns, oxygen levels, and airflow
In-Lab Polysomnography
- Gold standard, comprehensive evaluation
- Measures:
- Brain activity (sleep stages)
- Respiratory effort and airflow
- Oxygen saturation
- Limb movement and arousals
Key Metric: Apnea-Hypopnea Index (AHI)
- Mild: 5–15 events/hour
- Moderate: 15–30 events/hour
- Severe: >30 events/hour
2
Anatomical Mapping of the AirwayOSA is fundamentally an anatomical and functional problem. The critical question is: Where and why is the airway collapsing?
Drug-Induced Sleep Endoscopy (DISE)
- Performed under controlled sedation
- Allows real-time visualization of airway collapse during simulated sleep
- Identifies:
- Palatal collapse
- Lateral pharyngeal wall collapse
- Tongue Base Obstruction
- Epiglottic involvement
This is one of the most important tools in precision surgical planning.
3D Imaging & Structural Analysis
High-resolution CT or cone-beam imaging evaluates:
- Nasal airway obstruction
- Septal deviation and turbinate hypertrophy
- Soft palate length and thickness
- Tongue volume and position
- Skeletal structure (jaw alignment, airway volume)
3
AI-Enhanced AnalysisArtificial intelligence allows integration of:
- Sleep study data
- Imaging findings
- Endoscopic observations
- Outcomes from thousands of prior cases
This enables:
- Pattern recognition beyond human capability
- Prediction of surgical success rates
- Identification of optimal multi-level treatment strategies
- Continuous learning and refinement of care
We are shifting from reactive medicine to predictive medicine.
When Is Surgery the Right Option?
Surgery is not for everyone—but for the right patient, it can be definitive and life-changing.
Common Indications
- Intolerance or failure of CPAP therapy
- Anatomically driven airway obstruction
- Desire for a long-term solution rather than device dependence
- Multi-level airway collapse identified on evaluation
Importantly, surgery today is not a last resort—it is a strategic, evidence-based option.
Surgical Treatment Options
OSA typically involves multiple levels of obstruction, and the most effective approach addresses each of them in a coordinated way.
1. Nasal Surgery
Improves airflow and often enhances tolerance of other therapies.
Procedures include:
- Septoplasty
- Turbinate reduction
- Nasal valve reconstruction
Benefits:
- Improved breathing
- Reduced airway resistance
- Better CPAP tolerance (if needed)
2. Palatal Surgery (Soft Palate & Lateral Pharynx)
A common and critical site of collapse.
Expansion Sphincter Pharyngoplasty (ESP)
- Repositions the palatopharyngeus muscle
- Expands the airway laterally (not just front-to-back)
- Significantly improves airflow and reduces collapse
- Higher success rates and durability compared to traditional methods
Modern Uvulopalatopharyngoplasty (UPPP)
- Now reconstructive, not purely resective
- Focuses on tissue preservation and repositioning
- Reduced complications and improved functional outcomes
3. Tongue Base Reduction
Targets obstruction at the back of the tongue.
Options include:
- Radiofrequency tissue reduction
- Midline glossectomy
4. Hypoglossal Nerve Stimulation
A major technological advancement.
- Implantable device stimulates the hypoglossal nerve
- Moves the tongue forward during sleep
- Prevents airway collapse dynamically
- Controlled by the patient via remote
Ideal for:
- Moderate to severe OSA
- Patients intolerant of CPAP
- Favorable airway anatomy on DISE
5. Skeletal Surgery (Maxillomandibular Advancement – MMA)
Among the most effective treatments available.
- Moves the upper and lower jaws forward
- Expands the entire airway (nasal → hypopharynx)
- High success rates, especially in severe OSA
Precision Over Guesswork
Modern sleep surgery is defined by:
- Individualized Planning - No "standard operation" each plan is patient-specific.
- Multilevel Treatment - Addressing all sites of obstruction simultaneously or in sequence.
- Data-Driven Decision Making - AI and large-scale outcomes guide strategy selection.
- Functional + Aesthetic Balance - Particularly important in nasal and skeletal procedures.
What to Expect
Before Surgery
- Comprehensive consultation and history
- Sleep study review
- Imaging and airway evaluation
- Clear, individualized treatment plan
After Surgery
- Many procedures are outpatient or short-stay
- Recovery varies:
- Nasal surgery: relatively quick
- Palatal/tongue surgery: moderate discomfort
- Skeletal surgery: longer recovery but transformative results
- Gradual improvement in:
- Sleep quality
- Energy levels
- Cognitive function
Outcomes
When patients are properly selected and precisely treated, surgery can:
- Reduce or eliminate apnea events
- Improve oxygenation
- Restore restorative sleep
- Enhance cognition and productivity
- Reduce long-term cardiovascular risk
- Improve quality and length of life
Risks and Considerations
All procedures carry risk, which may include:
- Bleeding or infection
- Swallowing or speech changes (usually temporary)
- Residual or recurrent OSA
- Need for staged or additional procedures
A thoughtful, experienced approach minimizes these risks.
The Future of Sleep Surgery
We are entering a transformative era:
- AI models predicting outcomes before intervention
- Fully dynamic airway imaging
- Integration of wearable data and longitudinal monitoring
- Increasingly minimally invasive yet highly effective procedures
This is not theoretical—it is actively reshaping patient care today.
Final Thoughts
Obstructive Sleep Apnea is highly treatable—but it requires expert evaluation and a tailored strategy.
If you have struggled with CPAP or have been told that no other options exist, that is often no longer true.
With modern diagnostics, advanced surgical techniques, and AI-guided planning, we can now offer treatments that are:
- Precise
- Durable
- Personalized
- Life-changing
Next Steps
If you suspect OSA or are exploring treatment options:
- Undergo a formal sleep evaluation
- Seek a comprehensive airway assessment
- Consult with one of our experienced specialists in advanced, multi-level sleep surgery
Your airway is unique. Your treatment should be too.
